If you are currently seeking APP opportunities, create a profile on DirectShifts and update your preferences to receive AI matched job alerts. Click on the links below to apply for openings with healthcare leaders.
- Flexible Remote Psychiatric Mental Health Nurse Practitioner PMHNP- AZ
- Flexible Remote Psychiatric Mental Health Nurse Practitioner PMHNP- TN
- Contract Role | Operating Room Nurse | New York
- Full time with benefits |100% Remote | PMHNP| PA
- Immediate Start | PACU RN | NYC
Clinics generally consider four sources to determine APP salary:
- Going market rate based on internet search.
- Information from peers.
- Salaries paid to current APRNs or PAs at the practice.
- Their own intentional compensation plan based upon business model.
The most important takeaway for APRNs and PAs who receive an offer from a clinic is to use reliable salary data and negotiate in order to achieve a competitive salary.
Hospitals generally establish salaries by tiers. For example, Tier 1 may represent a base salary for a Monday through Friday schedule, Tier 2 will then add a fixed dollar amount for weekend days and evenings, and Tier 3 adds an additional dollar amount for 24/7 coverage.Each tier can represent a $3,000 to $5,000 difference. Additionally, many hospitals adjust base amounts by years of experience. For example, some hospitals pay new graduate APRNs for years of RN experience at a rate of 1 year of APP experience for every 2 years of RN experience, with a cap generally at 10 years of RN experience. The salary differential given for each year of experience can vary by role and is included in the chart below.
The data in the 2021 Salary Guide aligns with Central United States, make the following adjustments by location:
- Salaries in the Midwest and southeast have increased over the last two years and are represented by the salary data.
- In Northern California,salaries are up to 46% higher.
- In Southern California, the Seattle area, and New York, salaries are approximately 22% higher.
- In the Southeast and Northeast,salaries are approximately 8% lower than the salary results.
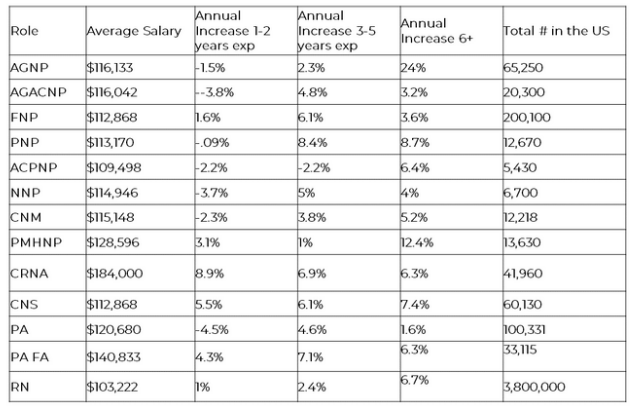
Why did some salaries decrease?
The simple answer is COVID. According to Becker's Hospital Review, "About 40 percent of respondents reported dips in their overall income, and 31 percent reported lower number of hours worked." For Acute Care PNPs (ACPNPs), salaries decreased with experience,which is most likely attributed to the number of hospitals that did not provide a salary increase. In particular for this role, children's hospitals were hit hard, losing as much as $40 million a month during the height of COVID.
Reflections on the results:
Primary care NPs are catching up to Acute Care NPs in salary. We did not see an increase in bonus plans, which means that salaries are going up for primary care.
PA newer provider salaries fell. Due of the large number of furloughed providers, this is not surprising. PA average salaries remain higher than most of the NP salaries, with the exception of CRNA and PMHNPs.
PA First Assist providers continue to receive substantial annual increases despite operating room shut downs. Many hospitals recognized that they needed to get the ORs open quickly, therefore continuing to employ and provide increases were in their best interest to keep this valuable workforce.
The average Salary for APPs is $120,973.
How to ask for incentive pay for APRNs and PAs
As Advanced Practice Providers (APPs,including APRNs and PAs) you have difficult, yet rewarding jobs, and deserve to be paid well for your work. The more you know about the salary structure, the better your ability to discuss alternatives. The cost of turnover for an employer is 2.5 times the cost of compensation, so it is worthwhile for employers to pay APPs well. To ask for incentive pay, APRNs and PAs need to start by gathering information.
Discuss with your employer their approach to salary. Understand salary structure - what is the range for your role? What is the max /cap salary for your role at the institution? Explore expected salary increases. Do they offer them? Why or why not? Does the organization provide annual raises? What is the average percent increase? Does your employer provide inflation or merit based raises, or a combination of both? If it is merit based, what is the criteria for earning your raise? Does your organization regularly assess and provide market adjustments? For example, if the organization provides an annual percent raise, but it is lower than salary increases throughout the rest of the market, then overall salaries will be lower than other places. How will they account for this discrepancy? Ask your employer if there is consideration for a base plus bonus model based on productivity. Download from here for reference.
Gather and ask for objective data of your performance measures (i.e. number of patients seen, billing, collections, and even patient satisfaction). You can also ask for visibility into other providers in the practice or to benchmark your practice against national data.Visibility can change behavior for the better when providers realize they are behind their colleague's measures. When individuals are aware that their work is being observed and that their performance is impacting institutional revenue,their productivity and the quality of their work improves. Then, ask to use this information to set up a base plus a bonus pay model. Use your current salary as your base and then ask for a percentage of your revenue based on your productivity. Many APPs have found that they are actually the highest producer in the office once they receive visibility.
You can present, as an alternative, a straight inflation based annual increase such as 2%. However, this is actually riskier for the practice because it commits them to a fixed salary no matter how much you produce. A base plus a bonus means that you will only be paid when you are producing more than your base. It also helps the employer to know that you are incentivized to code, write accurate and thorough notes, and work efficiently to see patients. Presenting this alternative and then advocating for a base plus a productivity based bonus is an effective way to negotiate for an incentive salary model.
All APPs should consider advocating for incentive pay. If you are considering talking with your employer about salary at your next annual review, start by:
- Looking up salary data on this report.
- Finding your advocate, APP leader, or other mentor.
- Learning about who the decision makers are, discussing with them the need for a raise or market adjustment, and then engaging them as your advocates.

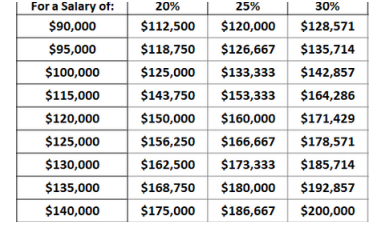
Total Compensation Calculation Table
Each cell represents total compensation,which is Salary plus a percent of the total Compensation allocated to benefits.Find your nearest salary on the left and your total compensation in the cell under the total amount of benefits you receive as a percent of your compensation (below).
Average Pediatric Nurse Practitioner (PNP) Salary:
Average PNP salary -$109,498.
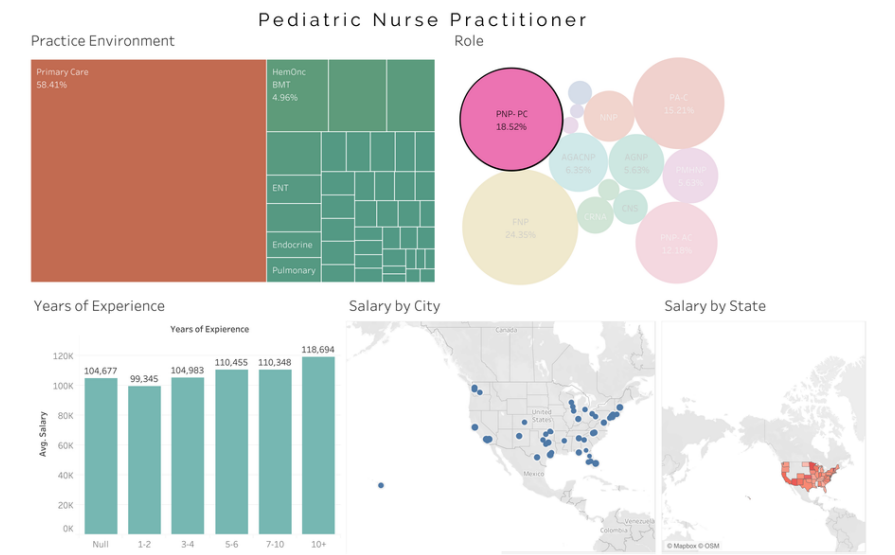
Average AC PNP salary- $114,946.
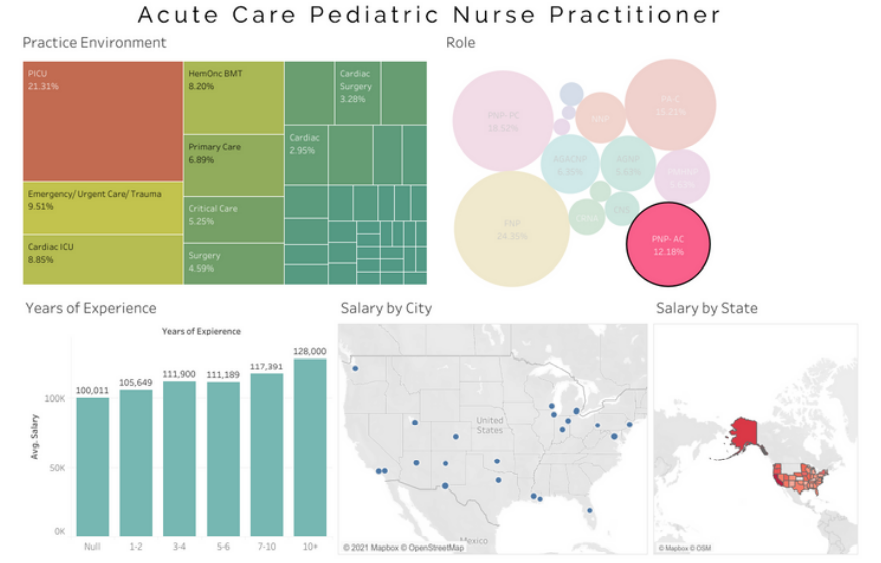
Average AGNP salary -$116,133
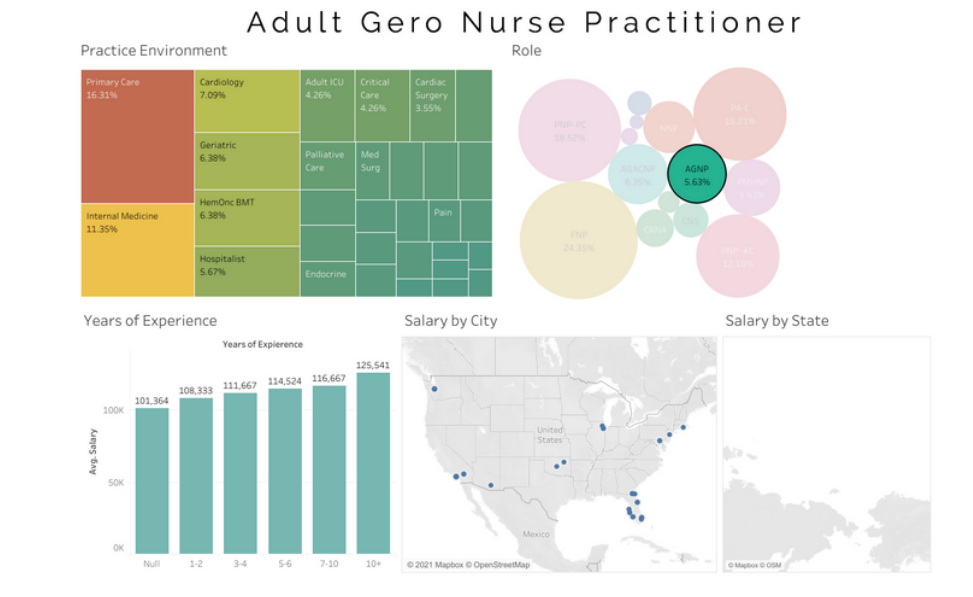
Average AGACNP salary- $116,042
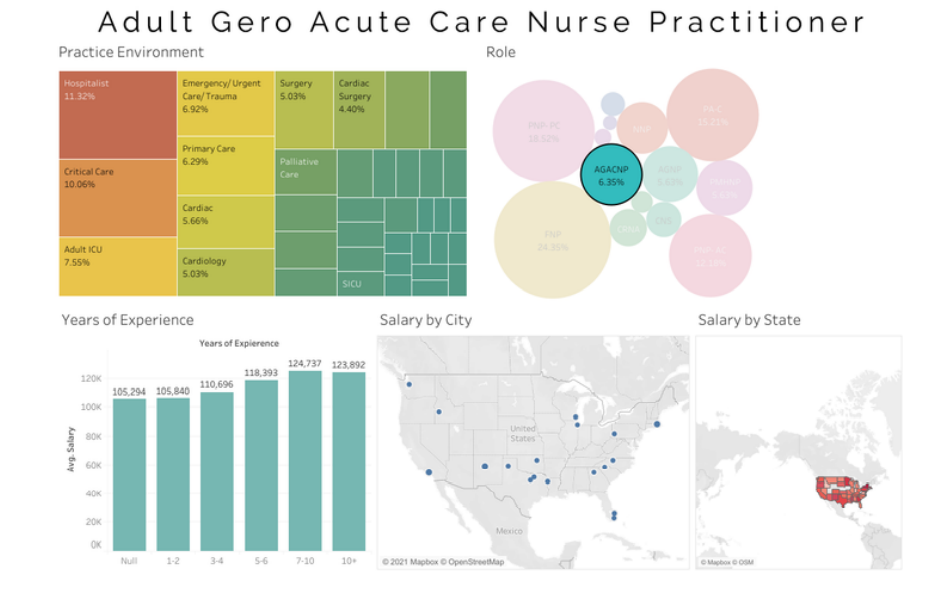
Average Family Nurse Practitioner (FNP) salary - $113,103
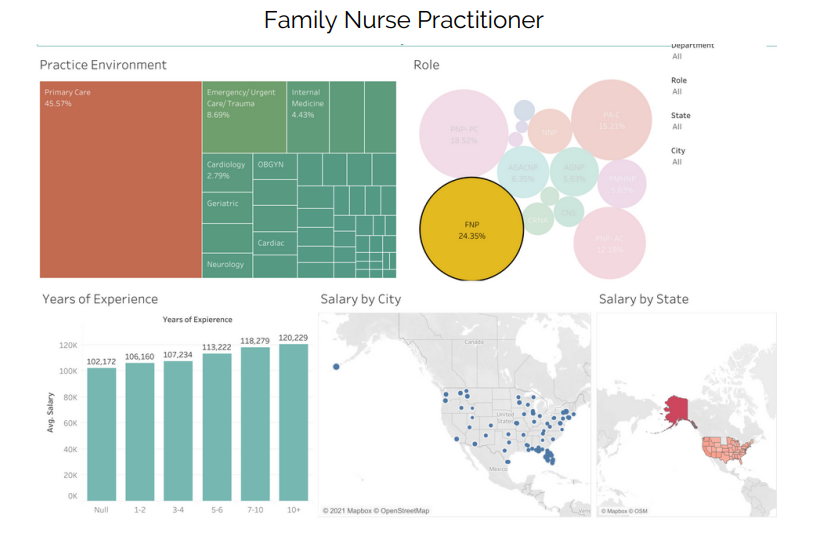
Average Neonatal Nurse Practitioner (NNP) salary - $121,716
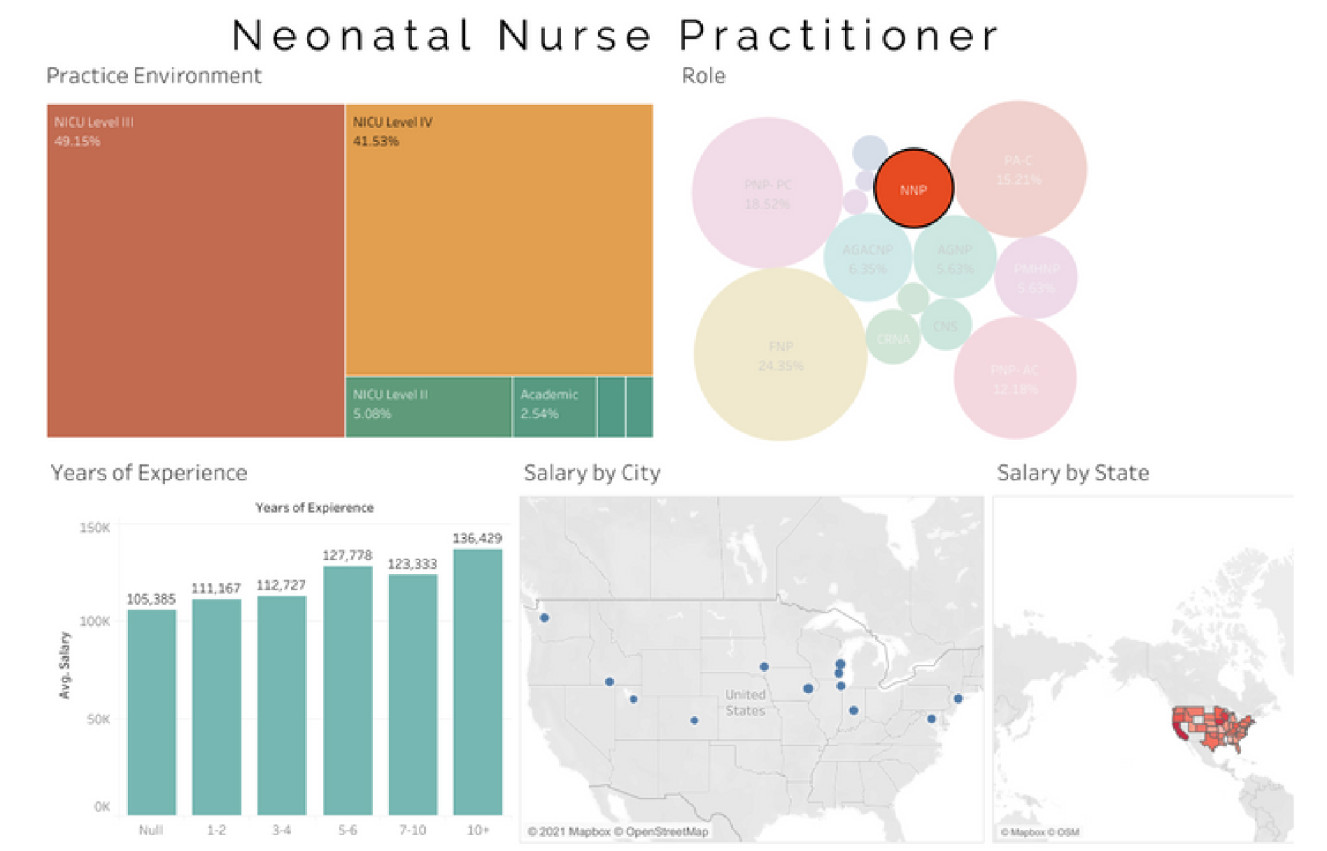
Average Certified Nurse Midwife (CNM) salary - $115,148
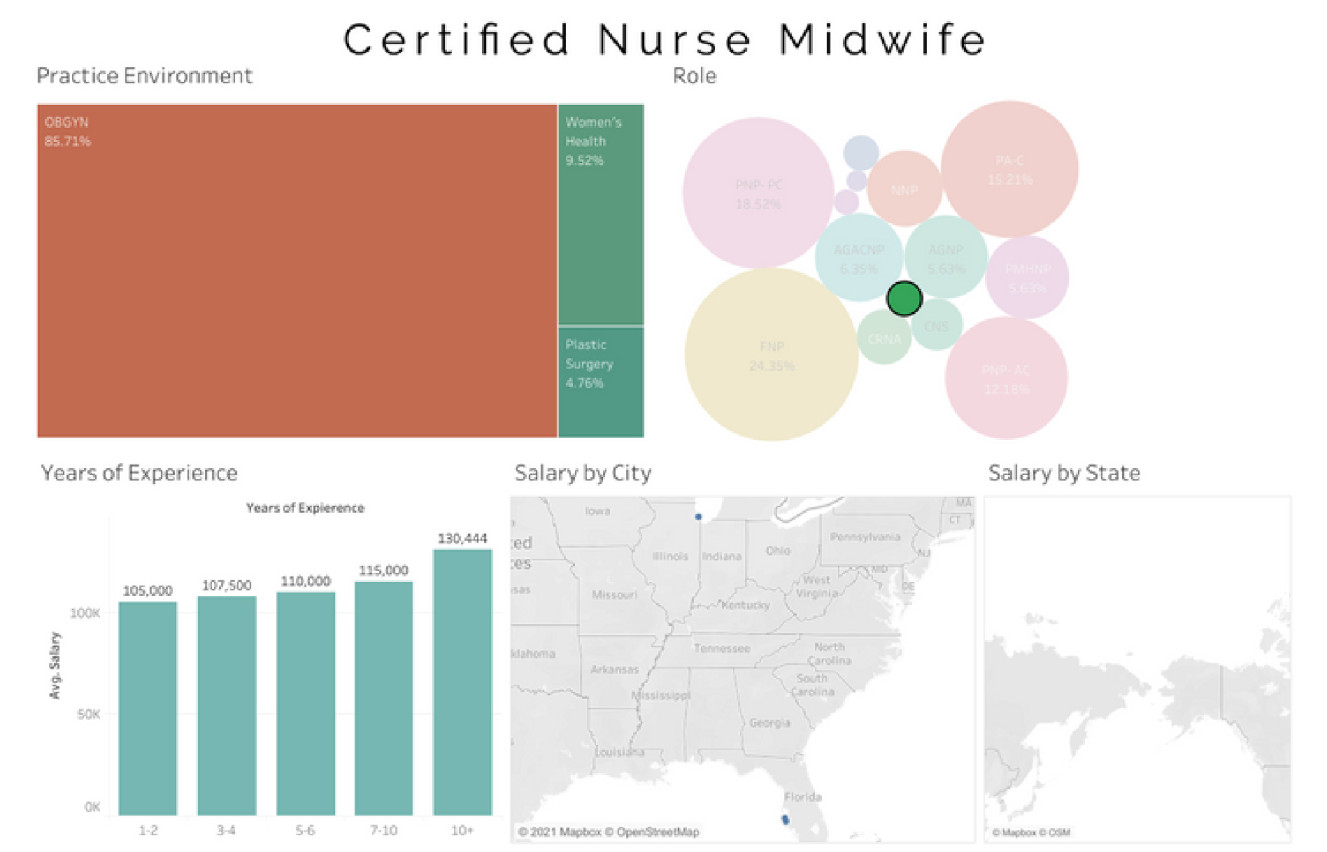
Average Certified Registered Nurse Anesthetist (CRNA) salary - $184,000
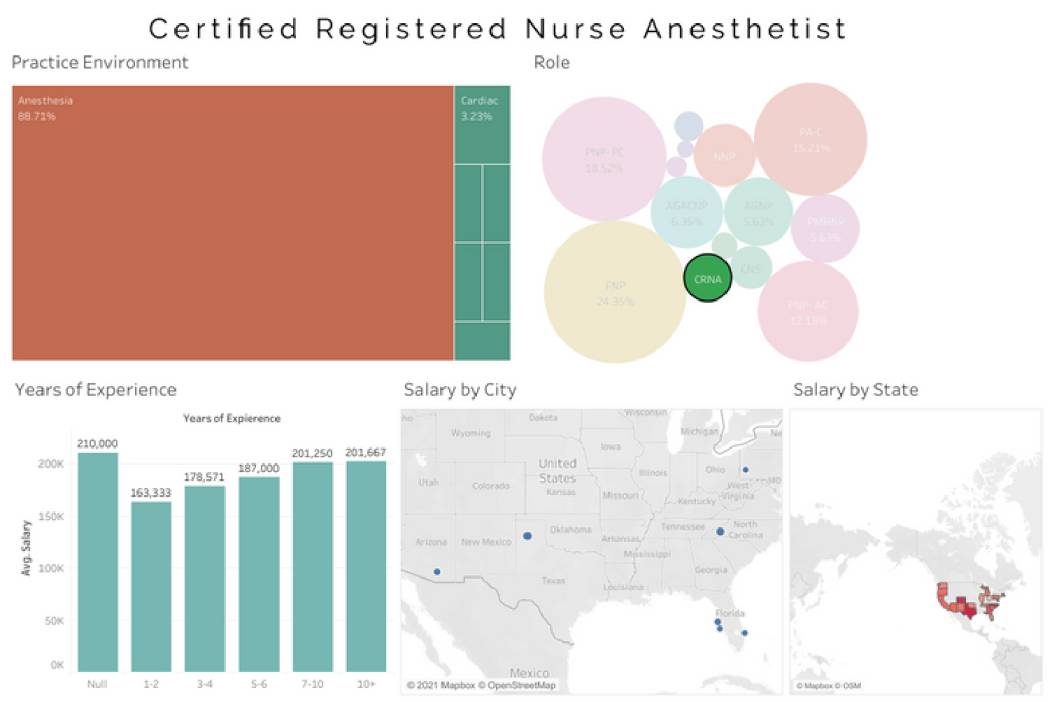
Average Psychiatric Mental Health Nurse Practitioner (PMHNP) salary - $128,596
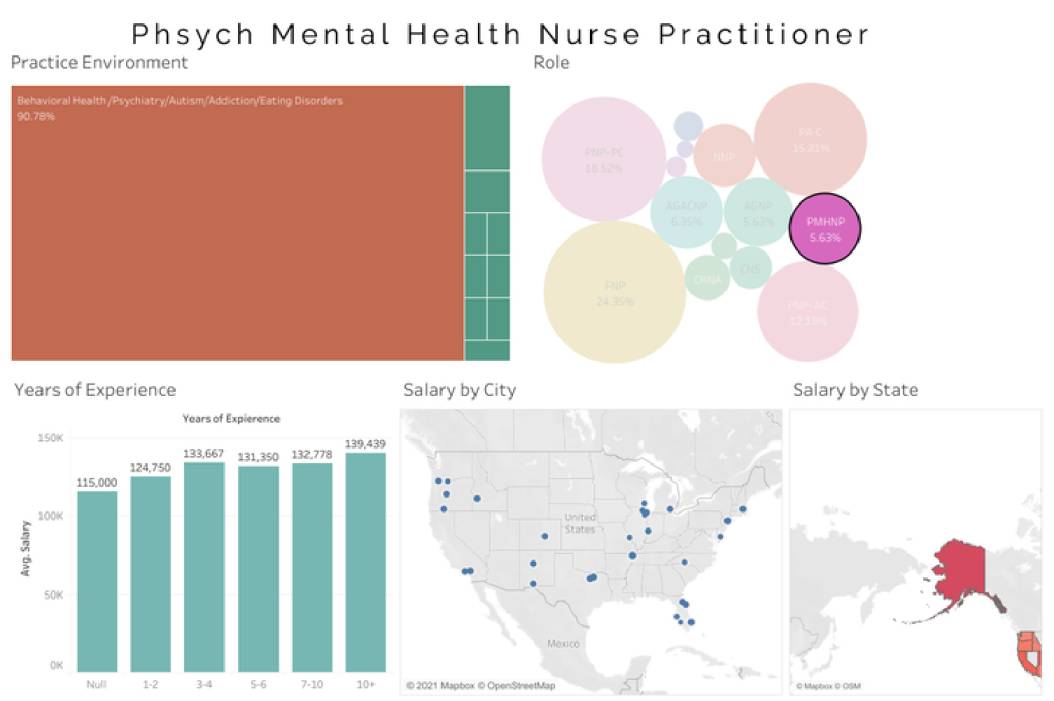
Average Woman's Health Nurse Practitioner (WHNP) salary - $105,000
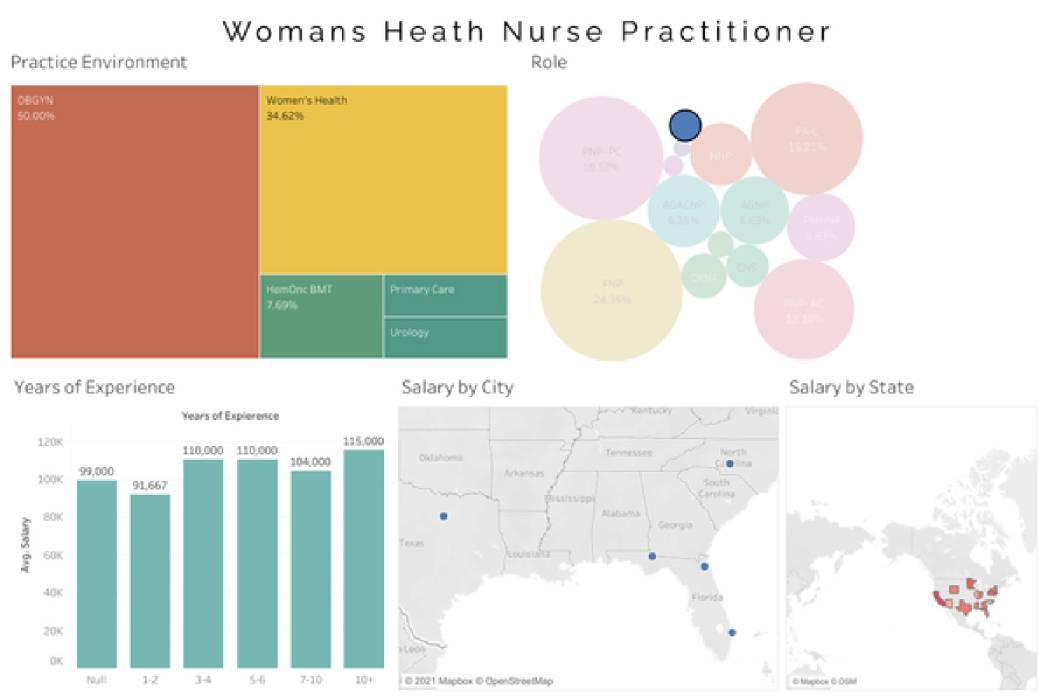
Average Nurse Practitioner Registered Nurse First Assist (NP RNFA) salary - $124,167
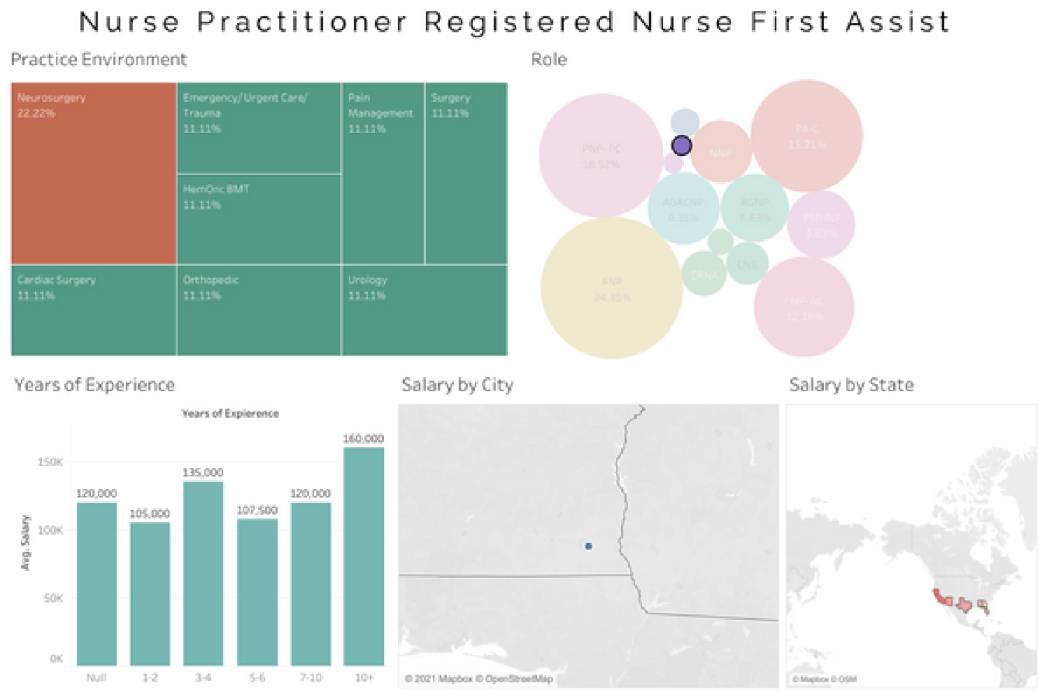
Average Clinical Nurse Specialist (CNS) salary - $112,868
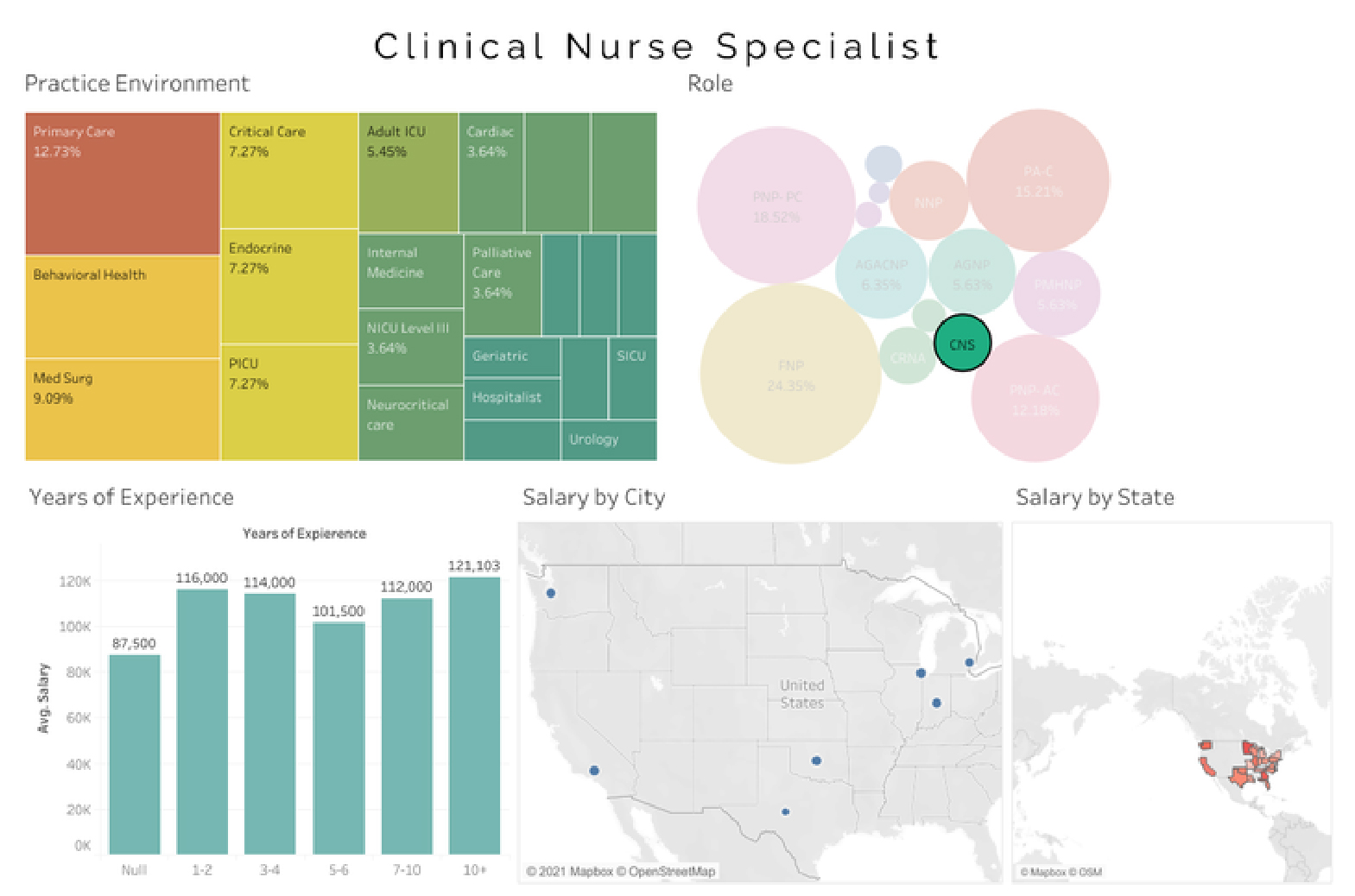
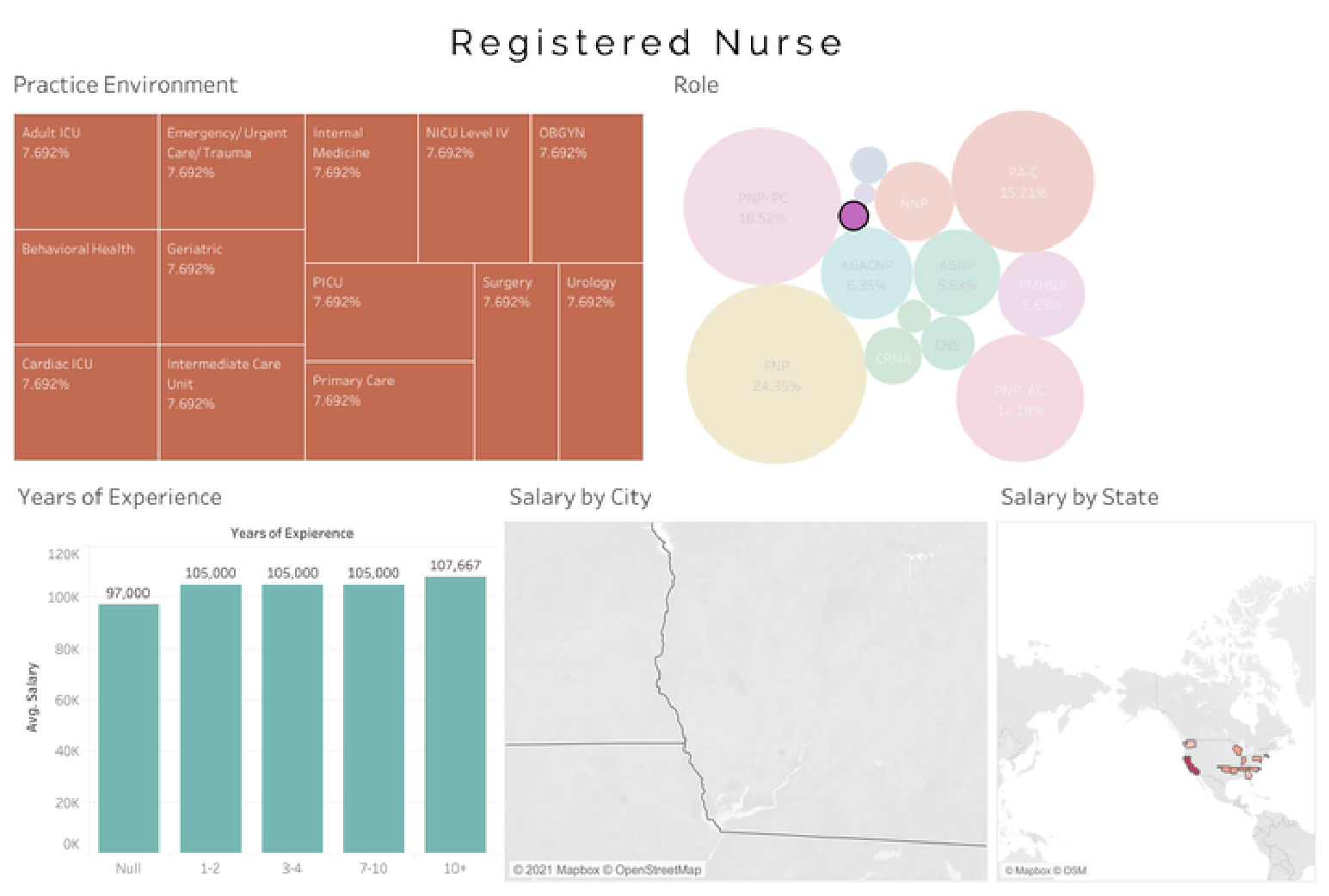
Average Registered Nurse (RN) salary - $103,223
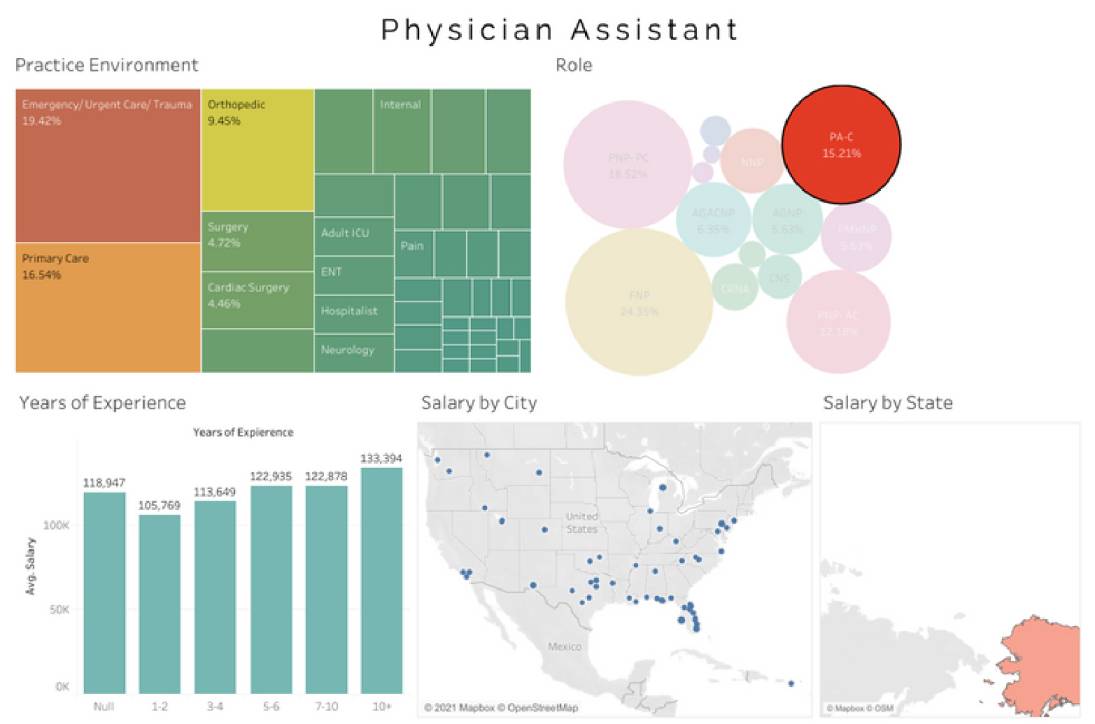
Average Physician Assistant (PA-C) salary - $120,680
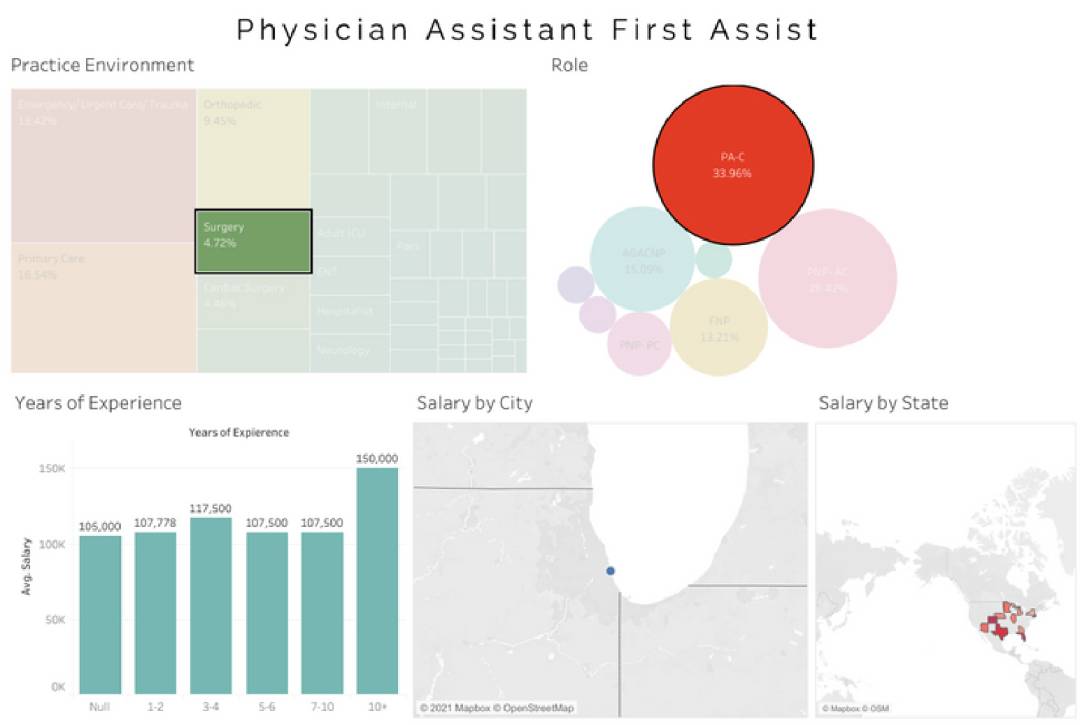
Average Physician Assistant First Assist (PA-C First Assist) salary - $127,253
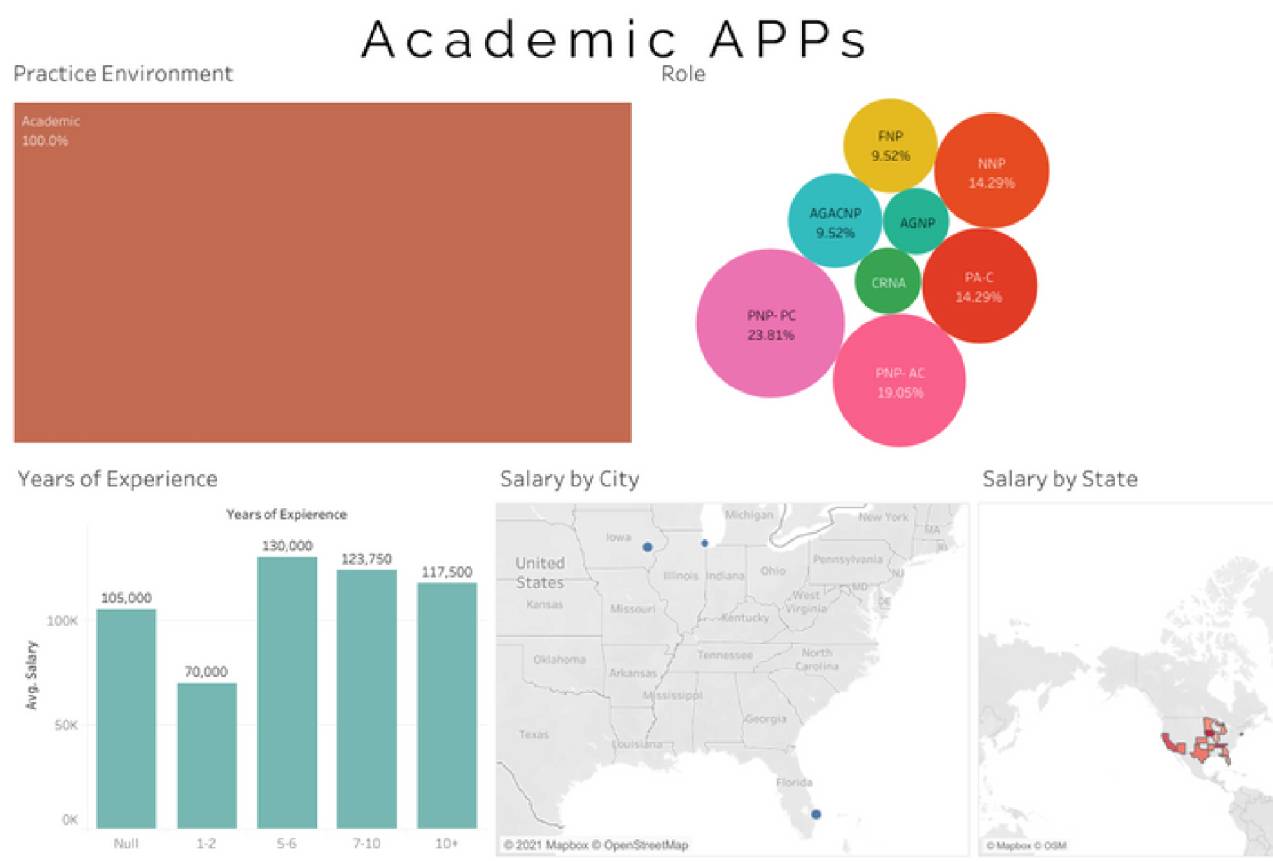
Average academic APP salary - $109,000
Additional Information:
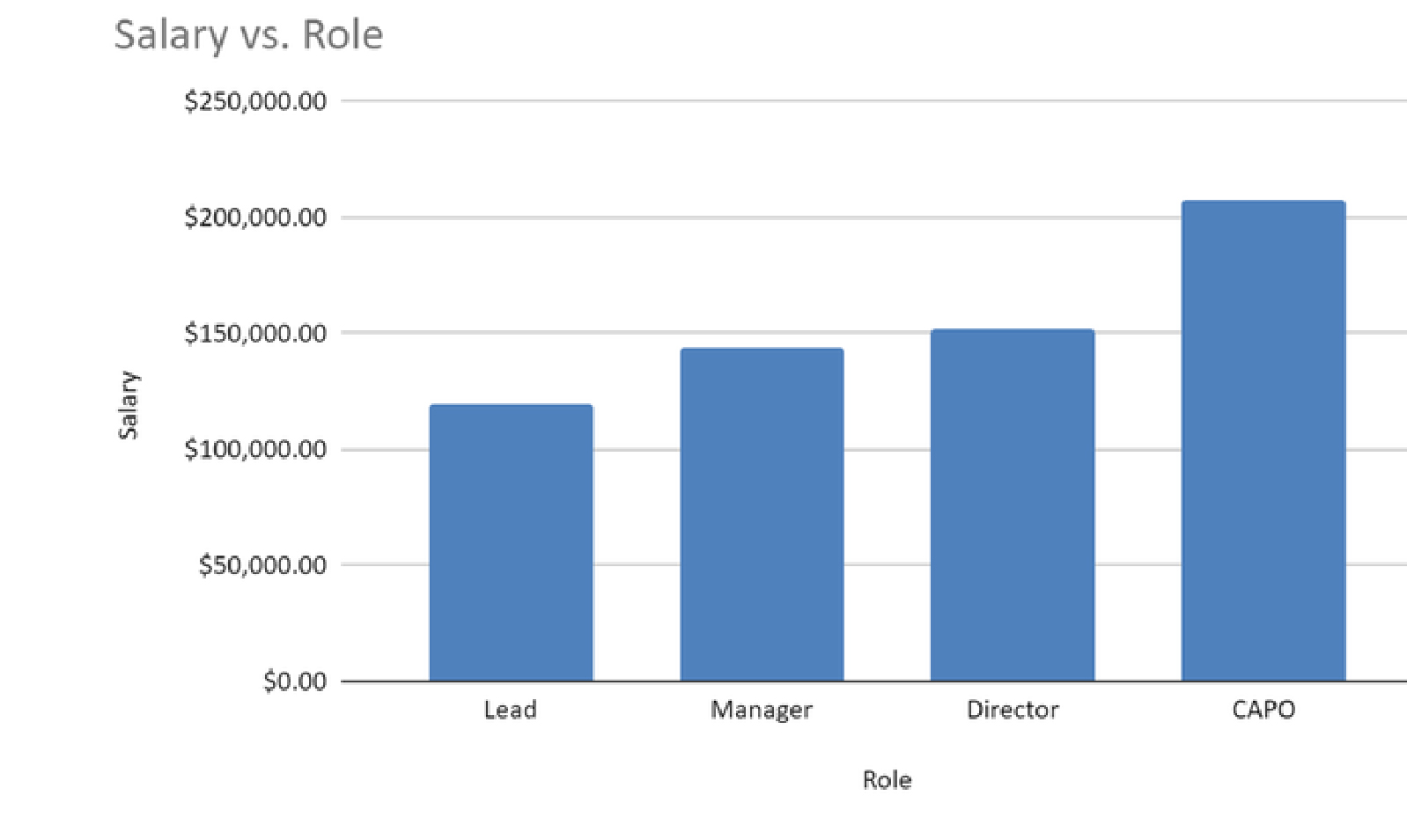
- Salaries are higher for CRNA Managers: CRNA Manager = $225,000
- 30% of Managers receivedbonuses of 5-15%
- 35% of Directors and Chief Advanced Practice Officers (CAPOs) received bonuses of 5-20%
Leads:
- Salary = APP salary for clinical responsibilities plus 5% additional salary for the leadership role.
- Perform evaluations, disciplinary duties, and manage scheduling 80% clinical & 20% administrative.
Managers:
- Salary = APP salary for clinical responsibilities plus 10% additional salary for the leadership role.
- Collaborate with nursing and physician leadership to achieve the goals of the service line, practice,or department.
- Create recruitment and retention strategies, including meeting with the APP teamto understand their needs.
- Implement professional advancement models and assess APPs toensure they practice within their scope of practice.
- Work with APP leadership to capture andimprove billing and to implement productivity dashboards. 40% clinical & 60% administrative.
APP Leadership: Responsibilities and Structures
Leadership structures can be built from the bottom up or top down. A bottom up build means that the organization hires APP leads, and then managers, and eventually a director or Chief Advanced Practice Officer (CAPO). A top down approach is when the organization starts by hiring a Director of Advanced Practice or Chief Advanced Practice Officer (CAPO) and supports that person as they build out leaders, such as managers and leads over service lines. There is organizational variation regarding APP leadership and support for the roles through salaries, titles, and administrative time.
Role of an APP Leader:
- Streamline reporting structures that provide clarification on roles and professional advancement within the organization.
- Standardize processes for hiring, credentialing, billing and orienting new APPs.
- Build APP professional advancement models.
- Improve recruitment and retention.
- Centralize budgeting and resource allocation, productivity measurement,clinical quality, and patient care.
- Anticipate and effectively respond to needs and changes in the practice environment.
Reporting Models for APP Leadership:
The first is reporting to the Chief Nursing Office (CNO), however the challenge being that PAs do not fit well within that model and having a single reporting structure can be beneficial. The next model includes reporting to the Chief Medical Officer (CMO). Generally,APP leaders align most with this structure and find it supportive.The final model is through the Chief Executive Office (CEO) or Chief Operating Office (COO), a model in which some find the highest level of empowerment and support within the organization. However,a downside of this structure may be that these individuals do not have a clinical background.
This report was originally published on Melnic by Jill Gilliland. Melnic was recently acquired by DirectShifts.
.png?width=50&height=50&name=Cube-Logo-150x150%20(1).png)
May 30, 2023


Comments